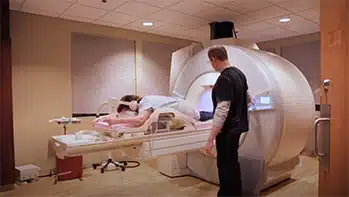
Breast MRI
Breast MRI is a powerful tool in diagnosing and staging breast cancer, as well as evaluating silicone breast implants. It can detect very small cancers, including those that cannot be picked up with mammogram or ultrasound.
Breast MRI is typically used for:
- Screening for breast cancer in women who are at a high risk for the disease. Women at high-risk often alternate between breast MRI and mammography as part of regular screening.
- Diagnosing breast tumors. Breast MRI may identify a small mass within a woman’s breast better than a mammogram or ultrasound.
- Determining the size of the tumor and extent of the spread after an initial breast cancer diagnosis. This is called staging the cancer.
- Monitoring the effectiveness of chemotherapy.
- Monitoring the tissues around the area where cancerous tumors or tissues were removed by surgery or chemotherapy.
- Guiding breast biopsies.
- Evaluating silicone breast implants for rupture.
What You Need to Know
The American Cancer Society (ACS) recommends that all high-risk women — those with a greater than 20% lifetime risk of breast cancer — have a breast MRI and a mammogram every year. For most women, these combined screenings should start at age 30 and continue as long as the woman is in good health. According to ACS guidelines, high-risk women include those who:
- Have a known BRCA1 or BRCA2 gene mutation.
- Have a first-degree relative (mother, father, brother, sister, or child) with a BRCA1 or BRCA2 gene mutation and have not had genetic testing themselves.
- Have a lifetime risk of breast cancer of 20-25% or greater, according to risk assessment tools that are based mainly on family history.
- Had radiation therapy to the chest for another type of cancer, such as Hodgkin’s disease, when they were between the ages of 10 and 30 years.
- Have a genetic disease such as Li-Fraumeni syndrome, Cowden syndrome, or Bannayan-Riley-Ruvalcaba syndrome, or have one of these syndromes in first-degree relatives.
The American Cancer Society also recommends that women at moderately increased risk of breast cancer — those with a 15-20% lifetime risk — talk with their doctors about the possibility of adding breast MRI screening to their yearly mammogram. According to ACS guidelines, this includes women who:
- Have a lifetime risk of breast cancer of 15-20%, according to risk assessment tools based mainly on family history.
- Have a personal history of breast cancer, ductal carcinoma in situ (DCIS), lobular carcinoma in situ (LCIS), or abnormal breast cell changes such as atypical ductal hyperplasia or atypical lobular hyperplasia.
- Have extremely dense breasts or unevenly dense breasts when viewed by mammograms
We encourage you to talk with your provider to find out what’s best for you.
Metal is not allowed in the MRI room because the magnetic field in the scanner attracts metal. Even some fabrics contain small amounts of metal, which can cause burns. That’s why we ask all of our patients to change into scrubs for MRI exams. You will be given a locker to store your clothes, and anything else you may have with you during your exam. You will be asked to remove any metal objects—even small ones—including jewelry, watches or hair clips.
The technologist will review the MRI safety checklist with you. This is to make sure you don’t have any metal in your body that could cause problems during the test. These could include:
- Hearing aids
- Body piercings
- Metal implants (such as valves, clips, stents, joints or limbs)
- Metal fragments (such as bullets, shrapnel or filings)
- Skin patches that contain metal
- Insulin pumps
- Implanted devices (such as pacemakers, neurostimulators, cochlear implants, drug pumps, cardioverter-defibrillator)
- Pins or screws
For our full MRI safety checklist, click here.
What to Expect
- We’ll give you a call before your appointment to talk through preparation instructions.
- Please provide the name, address and phone number of any facility where you have had a prior mammogram. If you have images from previous exams, please bring them to your appointment. Our radiologist may need these prior images for comparison in order to make an accurate diagnosis.
- Be sure to tell us if you are pregnant, nursing, or if there is a chance you may be pregnant.
- Contrast Breast MRI exams are ideally performed the week following your period.
- If sedation is requested, you should arrange for someone to drive you home.
- On the day of your exam, please arrive 15 minutes early for check-in.
- When you arrive, you will be led to a changing room and given a pair of scrubs to wear for your exam. You will be given a locker to store your clothes, and anything else you may have with you during your exam.
- The technologist will help position you on a cushioned table. An imaging device called a “coil” will be placed around the area of the body to be scanned. The coil acts like an antenna to help capture high quality images of your body.
- Once you are comfortably positioned, the technologist will go out of the room to run the scanner from a computer located directly next to the scanner suite, visible through the viewing window. The technologist will communicate with you throughout the exam and check to see how you are doing.
- When the scan starts, the table you’re on will move into the scanner so the technologist can capture images. It’s important to lie as still as possible during this part of the exam to help us capture clear images. You will hear “knocking” or “buzzing” sounds for a few minutes at a time.
- MRI contrast (a special dye that helps highlight your anatomy) will be administered through an IV placed in your hand or arm before your exam.
- When your scan is complete, you’ll be escorted back to the changing room so you can change out of the scrubs and back into your clothing.
- Once you have changed, your appointment is complete. You do not need to check out with the front desk when you leave.
- After the exam, your images will be sent electronically to one of our radiologists. This radiologist will review the information and send a report to your referring provider, typically within one to two business days.
- You should follow up with your referring provider to discuss your results.
- If you are premenopausal, it is best to have a Breast MRI 7 – 14 days after the start of your menstrual cycle.
- If you are taking hormone replacement therapy (HRT), you should be off this medication for 1-2 months prior to the exam.